Among the latest technological upgrades at Aspen Valley Hospital’s Breast Center, the SCOUT® radar location system transforms patient care at a critical time in a patient’s breast cancer journey.
Typically, surgeons perform lumpectomies after multiple diagnostic breast procedures, including a biopsy and a diagnosis of breast cancer. What was once an arduous process to prepare a patient for surgery is now a reduced to… a grain of rice. Enter SCOUT: A wire-free localization system that uses an implant about the size of a grain of rice for breast and soft tissue tumor localization. It can be implanted at the time of biopsy, or any other time before surgery that marks the biopsy site. The SCOUT® reflector system uses radar detection instead of the traditional wire and radiation system used by surgeons for generations to guide them to the tumor.
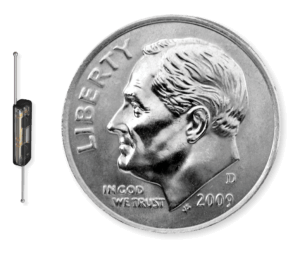
“This technology has been adopted by hospital systems across the country in just the last few years, and it has transformed the treatment and experience of patients and their clinicians,” says Dr. Betsy Brew, who performs lumpectomies at the Hospital. “Now we’re fortunate to be seeing the same benefits here at Aspen Valley Hospital.”
The system, in use at the Hospital since January, is used with both women and men who undergo lumpectomies. It also has FDA approval for targeting non-breast tissues such as lymph nodes.
A Game Changer for Patients
For patients, the SCOUT breast cancer treatment has made an otherwise stressful experience less so. Surgeons insert the grain-sized instrument with a needle, often at the time of biopsy and it remains in place until surgery. It can be used effectively throughout treatment, even during chemotherapy in advance of surgery.
- The SCOUT reduces the number of procedures patients go through on the day of their surgery. They no longer need to have a wire inserted into their breast right before surgery. This reduces stress and allows them to focus on their surgery.
- Because it is implanted at the time of biopsy or a different time before surgery, it allows the patient to schedule surgery weeks or even months after implantation.
- Implanting the SCOUT only requires a local anesthetic, allowing the patient to drive themselves to the Hospital. They also no longer need to restrict their eating before the procedure.
- The SCOUT can also improve cosmetic outcomes. It improves the surgeon’s ability to locate the tumor and choose the most direct route from the skin’s surface to the tumor, reducing the amount of impacted tissue.
- Before SCOUT, lumpectomies required coordination between the surgeon and the radiologist, who had to be on-hand for insertion of the wire. Now, only the surgeon and her support staff need to be present. This has markedly improved scheduling flexibility for the patient.
Improved Surgical Precision and Outcomes
Dr. Brew and the staff at the Breast Center have also benefited from the increased scheduling flexibility that patients experience. They no longer have to coordinate with other departments on the day of surgery. But that’s just a small part of the improvements they are seeing.
One of the biggest impacts is the surgeon’s ability to locate and remove the tumor with the least patient impact. How? Dr. Brew scans the breast using the SCOUT Guide. It emits infrared light and a radar signal providing real-time distance measurement, allowing her to detect the location of the reflector within 1mm of accuracy.
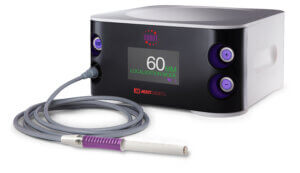
“It gives Dr. Brew the opportunity to select the shortest route from incision to tumor, which makes the surgery easier and improves the patient’s recovery experience,” says Kelly Fain, lead mammographer at Aspen Valley Hospital.
The SCOUT breast cancer treatment also improves surgical accuracy with patients who have undergone chemotherapy ahead of surgery. In many instances, chemotherapy shrinks the tumor so much that it is difficult to locate with traditional radiology. The SCOUT eliminates that challenge because of its location at the site of the tumor. Surgeons can use it to guide themselves to the precise location.
The ability to precisely locate tumors increases the probability of complete cancer removal and reduces the likelihood of follow-up surgeries. This creates a huge advantage for early-stage breast cancer patients, as well as those undergoing chemotherapy before their operation.
The technology gives Aspen Valley Hospital the ability to provide state-of-the-art treatment for patients close to home. It advances surgical outcomes and improves comfort and flexibility for the patient.
Aspen Valley Hospital’s Breast Center offers personal support for patients with Breast Navigator Heather Milne. You can reach Heather at 970.544.1420. Visit the Hospital’s Breast Center to learn more.

